Human papillomavirus, cervical cancer, and the vaginal microbiome
Background: Cervical cancer is the fourth most common cancer affecting women worldwide, primarily in low and middle-income countries [1]. In the United States, an estimated 13,960 new cases of invasive cervical cancer will be diagnosed and about 4,310 individuals will die from cervical cancer in 2023 [2]. Significant racial disparities in cervical cancer incidence and mortality are observed across the United States. In Arizona, Hispanic (8.8 per 100,000) and Native American women (8.4 per 100,000) experience the highest rates of cervical cancer [3].
Persistent high-risk genital human papillomavirus (HPV) infection accounts for approximately 99.7% of cases of cervical cancer [4]. Research shows that the cervicovaginal microbiota contributes to both HPV clearance or persistence and cervical cancer development and progression [5-7].
Areas of Interest:
Persistent high-risk genital human papillomavirus (HPV) infection accounts for approximately 99.7% of cases of cervical cancer [4]. Research shows that the cervicovaginal microbiota contributes to both HPV clearance or persistence and cervical cancer development and progression [5-7].
Areas of Interest:
- Health disparities in Hispanic women
- Health disparities in Native American women
- Microbiome-driven mechanisms of HPV persistence
- Cervicovaginal microenvironment related to HPV clearance and persistence (multi-omics)
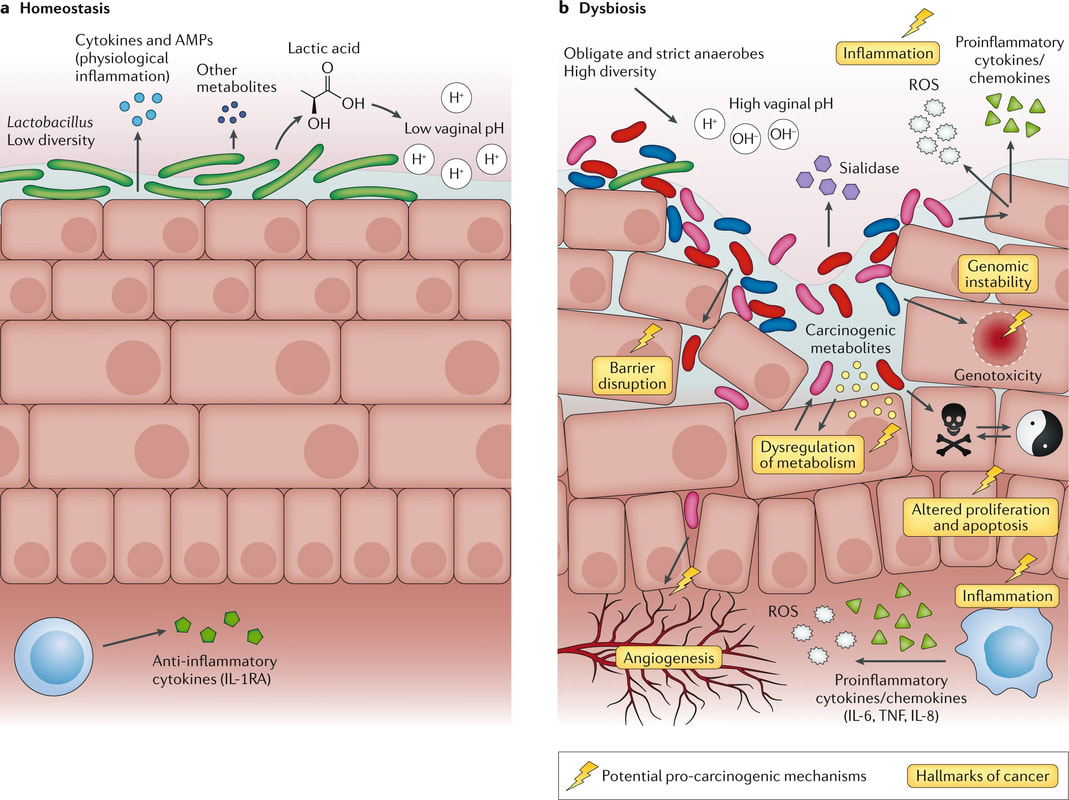
Effect of microbiota on mucosal homeostasis and hallmarks of cancer. Laniewski P, Ilhan ZE, Herbst-Kralovetz MM. The microbiome and gynaecological cancer development, prevention and therapy. Nat Rev Urol. 2020. PMID: 32071434
Projects
Related Projects: Studies conducted by the lab have characterized features of the cervicovaginal microenvironment, such as cancer biomarkers, immune mediators, genital inflammation, vaginal pH, and vaginal microbiome composition throughout cervical carcinogenesis. Ongoing projects are focused on raising cervical cancer awareness among Hispanic and Native American women as well as addressing cervical cancer health disparities.
Published Studies:
Published Studies:
- Morales CG, Jimenez NR, Herbst-Kralovetz MM, Lee NR. Novel vaccine strategies and factors to consider in addressing health disparities of HPV infection and cervical cancer development among Native American women. Med Sci (Basel). 2022 Sep 13;10(3):52. doi: 10.3390/medsci10030052. PMID: 36135837.
- Kaelin EA, Skidmore PT, Laniewski P, Holland LA, Chase DM, Herbst-Kralovetz MM, Lim ES. Cervicovaginal DNA virome alterations are associated with genital inflammation and microbiota composition. mSystems. 2022; e0006422. PMID: 35343798.
- Bokulich NA*, Laniewski P*, Adamov A, Chase DM, Caporaso JG, Herbst-Kralovetz MM. Multi-omics data integration reveals metabolome as the top predictor of the cervicovaginal microenvironment. PLoS Comput Biol. 2022; 18(2):e1009876. PMID: 35196323. * These authors contributed equally
- Bordeaux SJ, Baca AW, Begay RL, Gachupin FC, Caporaso JG, Herbst-Kralovetz MM, Lee, NR. Designing inclusive HPV cancer vaccines and increasing uptake among Native Americans—a cultural perspective review. Curr Oncol. 2021. 28(5):3705-3716. PMID: 34590604
- Laniewski P, Cui H, Roe DJ, Chase DM, Herbst-Kralovetz MM. Vaginal microbiota, genital inflammation, and neoplasia impact immune checkpoint protein profiles in the cervicovaginal microenvironment. NPJ Precis Oncol. 2020. PMID: 32802959
- Laniewski P, Ilhan ZE, Herbst-Kralovetz MM. The microbiome and gynaecological cancer development, prevention and therapy. Nat Rev Urol. 2020. PMID: 32071434
- Laniewski P, Cui H, Roe DJ, Barnes D, Goulder A, Monk BJ, Greenspan DL, Chase DM, Herbst-Kralovetz MM. Features of the cervicovaginal microenvironment drive cancer biomarker signatures in patients across cervical carcinogenesis. Sci Rep. 2019. PMID: 31089160
- Ilhan ZE, Laniewski P, Thomas N, Roe DJ, Chase DM, Herbst-Kralovetz MM. Deciphering the complex interplay between microbiota, HPV, inflammation and cancer through cervicovaginal metabolic profiling. EBioMedicine. 2019. PMID: 31027917
- Laniewski P, Barnes D, Goulder A, Cui H, Roe DJ, Chase DM, Herbst-Kralovetz MM. Linking Cervicovaginal immune signatures, HPV and microbiota composition in cervical carcinogenesis in non-Hispanic and Hispanic women. Sci Rep. 2018. PMID: 29765068
Grants and Funding
We would like to thank the Partnership for Native American Cancer Prevention (NACP) NCI, grant numbers U54CA143924 (University of Arizona Cancer Center) and the Flinn Foundation, grant numbers 1974 and 2244.
Sources
[1] World Health Organization. Cervical cancer. Published November 17, 2023. https://www.who.int/news-room/fact-sheets/detail/cervical-cancer
[2] American Cancer Society. Cervical Cancer Statistics. Published January 12, 2023. https://www.cancer.org/cancer/types/cervical-cancer/about/key-statistics.html
[3] Arizona Department of Health Services. Cervical Cancer in Arizona: 2000-2010. (2014) https://www.azdhs.gov/documents/preparedness/
public-health-statistics/cancer-registry/reports/cervical-cancer-in-az-2000-2010.pdf
[4] Okunade KS. Human papillomavirus and cervical cancer [published correction appears in J Obstet Gynaecol. 2020 May;40(4):590]. J Obstet Gynaecol. 2020;40(5):602-608. doi:10.1080/01443615.2019.1634030
[5] Mitra A, MacIntyre DA, Marchesi JR, Lee YS, Bennett PR, Kyrgiou M. The vaginal microbiota, human papillomavirus infection, and cervical intraepithelial neoplasia: what do we know and where are we going next? Microbiome. 2016;4(1):58. doi:10.1186/s40168-016-0203-0
[6] Brusselaers N, Shrestha S, van de Wijgert J, Verstraelen H. Vaginal dysbiosis and the risk of human papillomavirus and cervical cancer: systematic review and meta-analysis. Am J Obstet Gynecol. 2019;221(1):9-18.e8. doi:10.1016/j.ajog.2018.12.011
[7] Shi W, Zhu H, Yuan L, et al. Vaginal microbiota and HPV clearance: A longitudinal study. Front Oncol. 2022;12:955150. doi:10.3389/fonc.2022.955150
[2] American Cancer Society. Cervical Cancer Statistics. Published January 12, 2023. https://www.cancer.org/cancer/types/cervical-cancer/about/key-statistics.html
[3] Arizona Department of Health Services. Cervical Cancer in Arizona: 2000-2010. (2014) https://www.azdhs.gov/documents/preparedness/
public-health-statistics/cancer-registry/reports/cervical-cancer-in-az-2000-2010.pdf
[4] Okunade KS. Human papillomavirus and cervical cancer [published correction appears in J Obstet Gynaecol. 2020 May;40(4):590]. J Obstet Gynaecol. 2020;40(5):602-608. doi:10.1080/01443615.2019.1634030
[5] Mitra A, MacIntyre DA, Marchesi JR, Lee YS, Bennett PR, Kyrgiou M. The vaginal microbiota, human papillomavirus infection, and cervical intraepithelial neoplasia: what do we know and where are we going next? Microbiome. 2016;4(1):58. doi:10.1186/s40168-016-0203-0
[6] Brusselaers N, Shrestha S, van de Wijgert J, Verstraelen H. Vaginal dysbiosis and the risk of human papillomavirus and cervical cancer: systematic review and meta-analysis. Am J Obstet Gynecol. 2019;221(1):9-18.e8. doi:10.1016/j.ajog.2018.12.011
[7] Shi W, Zhu H, Yuan L, et al. Vaginal microbiota and HPV clearance: A longitudinal study. Front Oncol. 2022;12:955150. doi:10.3389/fonc.2022.955150